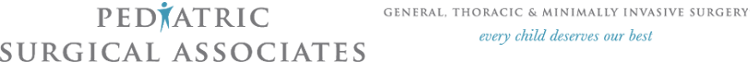Abdominal Pain and Pediatric IBD
 By Tiffany Linville, MD, FAAP, Levine Children’s Hospital
By Tiffany Linville, MD, FAAP, Levine Children’s Hospital
As a pediatric gastroenterologist, I see a wide variety of conditions that challenge our young patients and their families. We often see children and adolescents who struggle with abdominal pain, sometimes for months on end, with acute episodes that land them in the hospital. These parents remark, “She has always had gastrointestinal problems, but until now they’ve resolved on their own.” These are the times it’s worth getting a referral to investigate an inflammatory bowel disease diagnosis and determine a treatment plan to provide the best care for your child.
What is Inflammatory Bowel Disease (IBD)?
IBD is a chronic, autoimmune condition that causes inflammation throughout the gastrointestinal tract. The group of disorders includes the diagnoses of Crohn’s disease, ulcerative colitis (UC) and indeterminate colitis (IC). Twenty-five percent of patients with IBD present during childhood/adolescence and patients diagnosed earlier in life tend to have a more severe disease.
What causes IBD?
The exact cause of IBD is unknown, but there are genetic and environmental factors that contribute to its development. Research to delineate the exact genetic markers is ongoing. There is also continuing evaluation of the role of diet and antibiotics in development of these disorders.
What symptoms does IBD cause?
Typical symptoms of IBD include abdominal pain, diarrhea, blood in the stool and weight loss. Patients may also have vomiting, fever, growth issues and fatigue. Patients sometimes have extraintestinal manifestations of IBD. This can affect nearly any body system but the most common include joint pains or swelling, rashes and vision abnormalities.
Symptoms of IBD overlap with many other conditions. Sometimes patients have symptoms for a very short period, but other times the symptoms come and go for quite a while.
How is IBD diagnosed?
Laboratory testing is often quite helpful and may show anemia (low blood counts) and elevated markers of inflammation in the blood or stool. The official diagnosis of IBD requires endoscopies (EGD, colonoscopy and capsule endoscopy). Sometimes a special type of MRI or CT scan is also needed for diagnosis.
How is IBD treated?
Inflammatory Bowel Disease is a chronic illness for which there is no cure. Thankfully, many patients achieve remission with the use of medication, of which there are many. There is a significant amount of research being done and many new medications are being approved which is great news! All of the medications that are used aim to decrease inflammation. There are also diet options for those with a mild disease. Sometimes, surgical intervention is also necessary. The goal of treatment is to make the patient feel well and to heal any inflammation that is present.
A multidisciplinary approach to patients with IBD is important, as this disease affects our pediatric patients and their families immensely. Dieticians, social workers, psychologists, nurses and physicians work closely to ensure all aspects of our patients’ wellbeing.
Where can I learn more about IBD?
The Improve Care Now Network is a quality improvement database network connecting 110 Pediatric IBD centers across the world. The research and clinical information derived from the network has doubled the rates of remission for pediatric patients with IBD since its inception in 2006.
The Crohn’s and Colitis Foundation of America also has excellent resources for patients and families. There is a local chapter that has an annual walk and education day, in addition to many other activities for families to participate in each year.
Dr. Tiffany Linville is a board-certified pediatrician and pediatric gastroenterologist. She completed her general pediatric residency and later pediatric gastroenterology fellowship at the University of Florida. Dr. Linville is currently the director of the Pediatric Inflammatory Bowel Disease Program at Atrium Health’s Levine Children’s Hospital.
This blog was produced in partnership with Charlotte Parent. Click here for the original post and other parenting resources.
The Importance of Baby’s Head Shape in Development
 (Why A Blanket on the Floor Is Your Baby’s Best Friend!)
(Why A Blanket on the Floor Is Your Baby’s Best Friend!)
By Susan Klemm MS, OTR/L, Carolina Kinder Development
During the last 10 years, we have seen a steady increase in delayed milestones in infants. The increase in children whose heads are flattened also continues to rise. Many parents whose children are diagnosed with plagiocephaly or brachycephaly are commonly told, “it’s cosmetic,” or, “it will round out on its own.” While the condition might resolve with no intervention, it could also result in delayed acquisition of developmental milestones or even more serious issues, like jaw pain or sleep apnea. So, what is a parent to do?
A knowledgeable parent makes different and better decisions than a parent overrun with conflicting information from multiple sources. My hope is that this post provides important information about development and simple solutions to help your baby’s head shape.
What causes plagiocephaly and/or brachycephaly?
Plagiocephaly and/or brachycephaly have become more prevalent in back-sleeping babies, but it is also more common with prematurity, traumatic births, multiple births or other medical issues. A contributing factor is something called “container baby syndrome,” which refers to infants who spend lots of time in swings, car seats and other equipment, to the extent that it affects development and head shape. (It’s worth noting that expectant parents are often sold equipment falsely advertised as helping baby development.)
What are the complications of plagiocephaly and/or brachycephaly?
When mild, plagiocephaly will not impact later health or function. Sometimes, babies also have torticollis, which is a preference to turn in one direction. There is a higher incidence of cognitive and speech issues at the age of five in children who had plagiocephaly as an infant. Later, it can result in poorly fitting eyeglasses (if needed) and ill-fitting protective helmets for sports or occupations. When moderate or severe, plagiocephaly can lead to challenging conditions for adults that include temporomandibular joint dysfunction (pain with chewing or speaking), sleep apnea and vision problems.
What is the solution?
When it comes to development and head shape, education PRIOR to the birth of your baby is important! Further education, once the infant is born, is also highly useful. Unfortunately, this information is not readily available. Developmentally supportive head shape routines are not taught in prenatal classes. Most information in books, on Google, in online chat groups, or from a well-meaning day care provider, neighbor or grandparent is not sufficiently detailed or accurate.
Look for a short class designed specifically to teach developmentally supportive routines and what equipment or toys to purchase, and which to avoid. After the baby is born, go to a class on tummy time! These classes provide information on ways to hold your infant that support development and head shape, and other simple but important tips.
Finally, lying flat or side-lying on a blanket on the floor is truly a fantastic place for an infant when not being held. Unless directed otherwise by your pediatrician, have your baby sleep on a flat, firm surface, as recommended by the American Academy of Pediatrics. This is the safest place, as well as best for head shape and development.
My baby’s head is flat. Will she have to wear a helmet?
If you notice head-flattening or a preference to look in one direction, have your baby checked out by an occupational or physical therapist who specializes in this area. The best way to avoid a cranial band (helmet) and/or extensive therapy is to address concerns early and thoroughly. Oftentimes, one session is all that is needed to thoroughly assess the underlying issue and further educate the parent on the specifics of what their infant needs. For infants with more involved turning preference or head shape, a thorough evaluation may be followed by therapy for four to 16 weeks. A cranial band to reshape the skull is sometimes recommended. An occupational or physical therapist whose caseload includes mainly infants and also has expertise with manual therapy skill (craniosacral or myofascial release) is ideal.
Susan Klemm MS, OTR/L, founded Carolina Kinder Development in 2006 to prevent and treat head, neck and developmental issues in infants. The ongoing developmental and orthopedic issues during the early years are also part of their services.
This blog was produced in partnership with Charlotte Parent. Click here for the original post and other parenting resources.
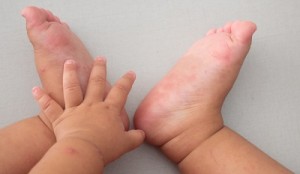
Common Questions About Conjunctivitis
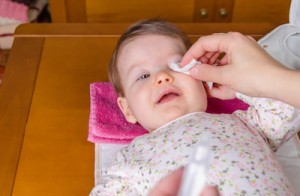 By Dr. Wissam Nadra, Lakeshore Pediatric Center, PA
By Dr. Wissam Nadra, Lakeshore Pediatric Center, PA
The American poet and philosopher, Henry David Thoreau once said, “The eye is the jewel of the body.” What do you do when that jewel starts itching, oozing and crusting over? If the pearly whites of your eyes start looking more like rubies, chances are you or your child has contracted conjunctivitis, otherwise known as “pink eye.”
Conjunctivitis is one of the most common infections of the eye and is usually easily treated, but it is very contagious! Here’s what you need to know.
What is conjunctivitis?
Conjunctivitis is an infection of the “whites of the eyes,” when the conjunctiva takes on a pink or red hue. It is a common eye infection in children under five years of age, easily spread in daycare and school. Parents and caregivers are also at risk of contracting conjunctivitis, so it is important to wash your hands thoroughly and make sure that children are instructed to do so.
Symptoms may include eyes that are reddened, watery, itchy or scratchy. Sufferers my also experience discharge from the eye(s) and crusting of eyelids or lashes.
Is conjunctivitis caused by a virus or bacteria?
Good question. In most cases conjunctivitis is a viral infection. It tends to be treated with a topical antibiotic ointment or eyedrops because viral eye infections can mimic bacterial infections.
Any person with a pink eye infection can infect other people even after starting topical antibiotics. In the majority of cases, you or your infected child can return to work or school 24 hours after starting your prescribed medicine.
Remember to discard any leftover topical medication after use! Do not use any leftover prescription eye drops from a previous eye infection, to avoid contamination.
When is it NOT conjunctivitis?
There are times when eye irritation can mimic classic conjunctivitis:
- Seasonal allergies may present with eye redness and irritation, with or without itchiness in the eyes.
- Irritant conjunctivitis from chemicals such as chlorine in freshwater pools can affect the eye(s).
- A foreign body in the eye can start with irritation but turn into a medical emergency.
We always recommend that you seek medical advice if you or a family member has pink eye. Any eye redness, irritation, persistence of pain or lack of improvement within 48 hours of starting any medication for this condition warrant seeking further advice from your medical provider. Of course, if you have any questions or concerns contact your pediatrician right away!
Wissam E Nadra, MD, MHA, FAAP, AIHM, holds a Bachelor of Science degree in Biology from the University of Southern California and received his medical degree from the American University of the Caribbean. He is a pediatrician and clinical director of Lakeshore Pediatric Center, PA, in Denver, NC.
This blog was produced in partnership with Charlotte Parent. Click here for the original post and other parenting resources.
Pediatric Surgery and Anesthesia Safety
 By Dr. Ashley McDonell, Providence Anesthesiology Associates
By Dr. Ashley McDonell, Providence Anesthesiology Associates
Whether your child’s upcoming procedure is elective or mandatory, we know that for many, the thought of surgery is scary.
For pediatric elective surgery, in children who are old enough to understand, we often explain that the administration process of general anesthetic is similar to flying an airplane:
- Takeoff — induction or “going to sleep”.
- Flying to a destination — the time during the actual surgical procedure.
- Landing — emerging from anesthesia in the recovery room.
Each of these three phases have specific safety concerns that are constantly monitored by your physician anesthesiologist and the anesthesia care team. Since most children do not have significant health conditions, their overall risk of a rare or unforeseen event from anesthesia is extremely low.
We often receive the following questions from parents:
What is a pediatric anesthesiologist?
A pediatric anesthesiologist is a physician trained to direct the presurgical and peri-operative care of infants and children. They are involved with the pre-operative evaluation, administration of anesthesia and post-operative care of pediatric patients. While the pediatric anesthesiologist may not meet you or your child face-to-face until surgery day, rest assured that he or she knows your child’s medical history and surgical plan. We carefully and methodically create an anesthetic plan to carry your child safely through their procedure.
Will my child receive an IV?
Most children are given an oral sedative about 15-20 minutes before the start of the procedure to calm them and facilitate separation from the parents. Once your child is relaxed, your anesthesia team will transport him or her to the operating room where they “go to sleep” breathing an anesthetic gas through a mask. When your child is completely asleep, an IV is started for the administration of fluids and pain medications. During surgery, most children continue to breath the anesthetic gas to keep them asleep.
Why is it important for my child not to eat or drink anything prior to anesthesia?
It is safest to give anesthesia on an empty stomach to decrease the risk of vomiting during surgery. If vomit goes into a child’s lungs, it can cause life threatening complications.
What if my child is sick the day of surgery?
It is important to call the surgeon’s office or pre-operative clinic to determine whether the child is well enough to undergo surgery. Depending on the severity of the illness and the nature of the procedure, we may delay anesthesia for when the child is well again. The pediatric anesthesiologist may want to evaluate the child the day of surgery to determine whether it is safe to undergo anesthesia.
When can I see my child after surgery?
We want to reunite you with your child as soon, as is safely, possible. Once your child is awakening and becoming aware, we will bring you to the bedside.
What can I expect after my child’s surgery?
Most children continue to be sleepy or confused after surgery, often caused by the side effects of most pain medications – not the anesthesia.
Is anesthesia safe for my child?
Overall, anesthesia is very safe. More common issues include nausea, sore throat and confusion after anesthesia. Typically, these effects resolve after a short period of time. In very rare cases, anesthesia can cause complications in children, such as abnormal heart rhythms, breathing problems, or an allergic reaction to certain medications.
Physicians and scientists have been studying the effects of anesthesia on the developing brain for two decades and continue to do research on the subject. Recently published research indicates that short, brief exposure to anesthesia in patients, age three years and under, is unlikely to cause long-term cognitive effects on behavior and learning. There are concerns about young children undergoing repeated or prolonged use of general anesthesia or longer surgeries (greater than three hours); however, many conditions require multiple anesthetics so the benefit may outweigh the risk.
Please be sure to talk to your child’s doctor, surgeon and/or anesthesiologist about any concerns. To learn more please visit: smarttots.org, pedsanesthesia.org and provanesthesiology.com.
Dr. Ashley McDonell works for Providence Anesthesiology Associates and is dedicated to providing the safest, most ethical care to meet the needs of every patient. Dr. McDonell graduated from UNC School of Medicine. She completed her residency at Maine Medical Center and a Pediatric Anesthesiology Fellowship at Seattle Children’s Hospital.
This blog was produced in partnership with Charlotte Parent. Click here for the original post and other parenting resources.
Parasomnias: When Sleep is Scary
 By Lili Poon, MD, Novant Health
By Lili Poon, MD, Novant Health
Night terrors, confusional arousals, sleepwalking and sleep talking: Most of us have heard of these or experienced them for ourselves. If you’re a parent, it’s likely that you’ve seen your child through one of these episodes. But what are they?
Parasomnias are unwanted or abnormal behaviors that occur during non-REM sleep. Though parasomnias can be concerning for a parent to witness and experience, they are not usually associated with negative health consequences. Often these conditions can be remedied or alleviated by helping your child get more sleep.
What are the most common parasomnias and what should you do, or not do, when your child is experiencing one? Let’s find out:
Sleepwalking
During a sleepwalking episode, the child may appear to be awake, wandering the home either in silence, mumbling, talking or yelling. As confusing as it can be to witness, the child is asleep and unaware they are sleepwalking. Sleepwalking can be dangerous if the right precautions are not taken to ensure a child’s safety, such as securing exterior doors, putting sharp objects out of reach and removing unstable furniture that they could bump into.
Confusional Arousals/Sleep Talking
Confusional arousals are variants of sleepwalking, where the child does not leave their bed. During a confusional arousal, the child may look awake and cry, talk, point or even arrange their stuffed animals on the bed. Sleep talking can range from mumbling, to clear conversations, to yelling out.
Night Terrors
Night terrors, also known as sleep terrors, can be the most disturbing to parents of all of the parasomnias. Unlike nightmares that occur during REM sleep, night terrors happen during non-REM sleep. During a night terror, the child may continue to be laying down or sit up, appearing frightened and scream or cry. Their eyes may be open, but they do not appear to improve with calming interactions of the parent.
Parasomnias can be relatively common. According to the National Sleep Foundation, parasomnias affect approximately 16% of children. They occur in people of all ages but are more common in children and most likely to happen during non-REM sleep, within the first few hours. Interacting with your child in this state may prolong the episode or worse, prompt an irritable, aggressive or even violent response from the child. If they are sleep talking, having a confusional arousal or night terror and have not left their bed, check on them and if they are safe, leave them alone. The more we interact, the longer and more violent the behaviors can get. If they are sleepwalking, try to gently redirect your child back to bed.
Parasomnias can occur when a child is not getting enough sleep for their age. Children require much more sleep than we do as adults, but don’t always get it. Though children ages five and under require 12 hours of sleep per night (in addition to daytime naps), most families set bedtimes permitting only eight to 10 hours of sleep. Many children who suffer from parasomnias see an improvement simply by improving their sleep duration, for their age.
It is a common misconception that children outgrow parasomnias as they get older. The parasomnias improve as their sleep requirement decreases with age to meet the sleep schedule implemented in the home. Parasomnias may recur in adulthood when unforeseen circumstances cause us to be sleep deprived. So remember, enough sleep is crucial to maintaining a good, quality sleep for children and those who care for them!
Dr. Lili Poon is a fellowship trained pediatric sleep physician and the pediatric sleep medical director at Novant Health in Charlotte, NC. Dr. Poon completed her fellowship at Case Medical Center in Cleveland, OH, and did her pediatric sleep training at Rainbow Babies Hospital in Cleveland.
This blog was produced in partnership with Charlotte Parent. Click here for the original post and other parenting resources.
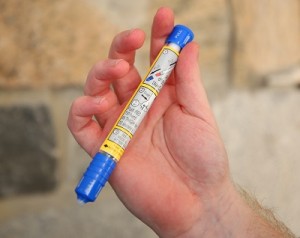
The Importance of EpiPens
 By Roy Lewis, MD, Charlotte Eye, Ear, Nose & Throat Associates
By Roy Lewis, MD, Charlotte Eye, Ear, Nose & Throat Associates
If you know someone with an allergy, chances are they’ve talked about needing an EpiPen. But what is an EpiPen and what does it do?
What is an EpiPen?
EpiPen is actually the brand name for a device that automatically injects epinephrine into someone having a severe allergic reaction, known as anaphylaxis. Epinephrine narrows the blood vessels and opens airways in the lungs, reversing severely low blood pressure, wheezing, hives and other symptoms. EpiPens are available in both adult and children’s doses.
Epinephrine is the first and most important treatment for anaphylaxis. While most commonly used for food or bee sting allergies, they can be used for any allergic reaction.
Auvi-Q is another brand name of auto-injectable epinephrine. Auvi-Q and EpiPens are not a substitute for medical treatment. If you have to use an EpiPen or Auvi-Q, seek medical attention afterward. Some patients with anaphylaxis will require more than one dose of epinephrine to resolve their reaction.
Auvi-Q and EpiPen Side Effects
Some side effects associated with epinephrine use include breathing troubles or severely high blood pressure. You may also experience an accelerated heartbeat, nausea, dizziness, tremors, or a headache. Some other medicines will affect an EpiPen, too. Discuss your other medications with your doctor before using an Auvi-Q or EpiPen.
Auvi-Q, EpiPens and Immunotherapy
Some patients with severe allergies receive immunotherapy. This is a regular series of treatments where patients are given gradually-increasing doses to increase their tolerance to allergens. In these cases, it is important for patients to have an Auvi-Q or EpiPen available.
Severe allergic reactions can be scary, and epinephrine injectors can be a good first treatment before receiving medical attention. But it’s important to remember that they’re not a replacement for proper medical care. Make sure you regularly discuss your allergy issues with your doctor and seek medical treatment when you need it.
This blog is for informational purposes only. For specific medical questions, please consult your physician. Dr. Lewis sees patients in CEENTA’s Mooresville office. To make an appointment with him or any of CEENTA’s ENT doctors, call 704-295-3000.
This blog was produced in partnership with Charlotte Parent. Click here for the original post and other parenting resources.
The Not-So-Obvious Facts of Hand, Foot, and Mouth Disease
By S. Chad Hayes, MD, FAAP
Hand, foot, and mouth disease (HFMD) is a common illness in young children and a frequent reason for a visit to the pediatrician. Like the other cause of preschool panic (conjunctivitis, or “pink eye”), HFMD is typically a mild illness that causes a lot more worry than it should.
This illness can affect people at any age, but it is seen most frequently in preschool-age children, most often in the late summer or early fall. It can be caused by several different viruses—usually strains of Enterovirus or Coxsackievirus. So while most children will develop long-lasting immunity after an infection, they can still get HFMD again if they are infected by one of the other strains.
This viral infection can cause painful blisters in the mouth and a rash that often shows up on the arms, legs, and buttocks, in addition to the places you already guessed based on the name. The rash can look like red spots, blisters, or bumps, and it’s usually not itchy or painful. Many kids will have a fever as well.
For the vast majority of children, HFMD will go away by itself in about a week without causing any major issues. The most common complication is dehydration, which can happen if a child refuses to drink due to the painful mouth blisters. Dehydration can usually be prevented by treating pain with ibuprofen or acetaminophen and encouraging fluid intake (popsicles count!). Rarely, children who are unable to stay hydrated will need to be admitted to the hospital for IV fluids until the illness gets better. Other than that, there’s usually nothing else to do, because we don’t have any magic to make HFMD go away faster.
One little-known complication of HFMD is the loss of fingernails and toenails within a few weeks of the infection. Fortunately, this condition called onychomadesis is relatively rare. Even more fortunately, nails tend to grow back normally.
The viruses that cause HFMD can be spread by saliva, but more often, they infect new people via the “fecal-oral route.” This is a method of disease transmission that involves swallowing poop particles—an event that occurs far more commonly than most of us care to imagine. If you have trouble understanding how this could possibly happen, try volunteering at a daycare for a couple hours. Or keeping a handwashing log in the bathroom at your favorite taco shop. Or just trust me.
The best way to prevent the spread of HFMD is by good handwashing and hygiene practices, especially in places like daycares or preschools that deal with a lot of dirty diapers. This is far more important and effective than excluding kids with HFMD from daycare or school, because these viruses can be shed in the stool for several weeks after the rash resolves. Additionally, some people can be infected with these viruses without developing any symptoms, while stealthily spreading it to anyone who comes into contact with them…or, well, their poop.
Many parents are surprised to learn that HFMD shouldn’t keep kids out of school or childcare facilities. If a teacher or administrator tells you differently, try referring them to the guidance published by the North Carolina Department of Health and Human Services, which specifically says that exclusion is not required.
While HFMD is usually a mild disease that resolves without treatment, there are a few rare complications, as well as several other illnesses that can have similar symptoms. So as always, if you have concerns about your child’s health, contact your pediatrician’s office. Sorting those things out is what we do best.
Dr. Hayes is a pediatrician at South Lake Pediatrics, Huntersville, an Atrium Health Levine Children’s practice. His writing can be found on his blog at chadhayesmd.com and in several other publications, including the Washington Post and Newsweek.
This blog was produced in partnership with Charlotte Parent. Click here for the original post and other parenting resources.
Your Child is Having a Medical Emergency, Now What?
 By Michelle Capizzi, MD, and Sara Steelman, MD
By Michelle Capizzi, MD, and Sara Steelman, MD
As career emergency medical physicians, we know an unexpected trip to the emergency department can be overwhelming and anxiety-inducing for you and your child. There are several things you can do to either avoid a visit to the emergency department or make your experience less stressful.
Don’t Panic!
While you may feel scared and out of control, your child needs you to be brave. You are your child’s greatest comfort and biggest advocate. It’s amazing to see how a parent with a calm and assuring presence can help a child during emergency evaluation and treatment.
Be Prepared
One of the best ways to minimize your fears is to be prepared before disaster strikes. Have a first-aid kit in the home, take a CPR class and learn the Heimlich maneuver. Keep the number to your pediatrician, local urgent care and poison control center nearby. The mental calmness that comes from knowing you’ve done the prep work if your child ever experiences a medical emergency is invaluable.
Monitor Fever
Any infant under 2 months with a fever of 100.4 degrees or greater (measured rectally), needs a laboratory evaluation and is best served in a dedicated pediatric emergency department. Most pediatric offices have a nurse triage line designed to help you determine where your child would best be served by talking through their symptoms. If the nurse triage line is not available to you, your local healthcare system’s advice line offers this same evaluation.
Call Poison Control
If you suspect your child may have ingested something but is acting normal and seems okay, we advise calling poison control first. The poison control center is very knowledgeable and may save you a time consuming and expensive visit to the emergency department. Some household ingestions can be managed at home, but if you do take a trip to the emergency department, bring what you suspect was ingested (medicines, cleaning supplies, etc.) with you, along with any medications your child takes on a regular basis. That will help us determine what we need to do for your child.
Be Patient
If you do need to go to the emergency department, explain the process to your child beforehand to help minimize fear. Care is prioritized based on how sick your child is and is not determined on a first-come, first-served basis. This can be hard for some children to understand. The waiting can be long and feel frustrating. If possible, leave siblings at home. Grandparents, aunts, uncles and cousins are great, but will not benefit in the evaluation and treatment of the child. One or both parents is really all that is needed.
Take Notes
Bring a pen and paper so you can take notes and write down the names of those caring for your child. If you are having trouble understanding a condition or diagnosis, ask your providers to draw or diagram. And yes, you can ask a million questions. We don’t mind.
Know that as pediatric emergency physicians, we have dedicated our professional careers to caring for sick and injured children. We love what we do. We love the resilient and open nature of children. Seeing a child get better and have a positive experience in our emergency department is why we come to work every day.
Michelle Capizzi, MD, is a board-certified pediatric emergency medicine physician with Novant Health Hemby Children’s Hospital Emergency Department. She has 20+ years of experience in pediatric emergency medicine and is a mom of five.
Sara Steelman, MD, is a board-certified pediatric emergency medicine physician and medical director of Hemby Children’s Emergency Department. She has 25+ years of experience in pediatric emergency medicine and is a mom of three.
This blog was produced in partnership with Charlotte Parent. Click here for the original post and other parenting resources.
Is My Doctor Speaking Greek?
By Maria Baimas-George, MD, and Daniel Bambini, MD
 You walk into a doctor’s office with your child. Your child is really sick and you’re scared. After all the tests are complete, the doctor walks in and proceeds to use words like appendicitis, leukocytosis, ultrasound, periappendiceal fat stranding, vestigial, laparoscopic, dermabond, etc. You try to keep up, but the more he speaks, the less you understand. Unfortunately, this can be common.
You walk into a doctor’s office with your child. Your child is really sick and you’re scared. After all the tests are complete, the doctor walks in and proceeds to use words like appendicitis, leukocytosis, ultrasound, periappendiceal fat stranding, vestigial, laparoscopic, dermabond, etc. You try to keep up, but the more he speaks, the less you understand. Unfortunately, this can be common.
Medical doctors go to medical school for many years to learn this language. Throat pain becomes dysphagia; an ingrown toenail becomes onychocryptosis; and bed-wetting is elevated to nocturnal enuresis. Doctors get accustomed to using fancy words when describing even the simplest of things and sometimes forget that this is not a language known to everyone. Even if a doctor does a great job of explaining a serious illness or painful prognosis, a parent’s understandable fear — maybe even shock — means he or she needs time to process and be ready to comprehend what is being explained.
When these things happen and parents do not speak up or ask questions, inevitably they turn to Dr. Google, and that’s where miscommunication gets even worse. The internet is a wonderful resource, but it can contain incorrect or contradicting information, which can be detrimental in effectively advocating for your sick child.
Pediatric surgeons spend a lot of time explaining complex medical issues to parents and children, and find that regardless of the topic or complexity, it is best to start from the beginning and try to tell a story. Let’s use appendicitis as an example.
What is normal?
We first explain what is normal and what the appendix does in the body. “Once upon a time, there was a healthy appendix that did nothing but nap like a cat…”
Where is it?
We explain the anatomy, what the appendix looks like and where is located. We also incorporate drawings for visual learners. (Unless you’ve dissected a human cadaver in an anatomy lab, it’s difficult to envision the location of the appendix.) For those who are not artistically talented, there are computer and tablet apps that work well.
What went wrong?
Next we explain why the appendix is hurting your child. (Appendicitis occurs when this small finger-shaped organ becomes infected.) We assure your child that there’s nothing he or she did to make the appendix become infected; it just happens. In rare cases the appendix ruptures (or pops) like a balloon!
How are we going to fix it?
It’s our hope that these stories have a happy ending, so that’s how we explain it. The standard treatment for typical appendicitis is a short, simple operation to remove the appendix. With very small, specialized tools and scopes, we can remove an infected appendix with a few small incisions.
If you are working with a medical professional who is speaking “Greek” to you, remember:
- It is OK to interrupt and say, “Hold your horses, that word makes no sense.”
- Don’t be afraid to interrupt and ask questions. Ask for more detail or a visual until you understand.
- Repeat it back. Tell the doctor what you think he or she has said.
- Take notes! We even have parents in the health care field do this when it’s their child who is the patient. When your child is hurting and you’re scared, nervous or overwhelmed, even your own medical training can take a back seat.
Maria Baimas-George, MD, MPH, is a surgical resident who works with and is mentored by Pediatric Surgical Associates at Carolinas Medical Center.
Daniel Bambini, MD, is a board-certified pediatric surgeon with Pediatric Surgical Associates in Charlotte.
This blog was produced in partnership with Charlotte Parent. Click here for the original post and other parenting resources.
How Safe are Trampolines for Children?
 By William T. Chirico Jr., OrthoCarolina
By William T. Chirico Jr., OrthoCarolina
The warm breezes of the summer months beckon children to play outdoors, burn off energy and get some fresh air. And in our modern era of video games, tablets and mobile devices, any alluring outdoor plaything that grabs kids’ attention will typically get parent votes, too.
But then your children see the neighbors’ kids jumping on their new trampoline, and come running to ask you if they can jump too. Sometimes the group on the trampoline is more than just one or two in number, and suddenly you envision a horde of ten kids screaming with delight, bouncing in close proximity. The what ifs race through your mind as your anxiety levels start to spike. As a parent, how do you respond?
As a physical therapist I never want to discourage children from getting exercise or that feeling of freedom and fun that comes from the joy of jumping on a trampoline. So here’s the low down about the injuries that typically happen and how to best avoid them.
It’s probably not a surprise to hear that most trampoline injuries happen as the result of children colliding with one another, tripping on the trampoline springs or frames, falling off the trampoline or attempting stunts that go awry. Most injuries happen to the leg or foot, followed by the arm or hand, and then the head/face/neck/shoulder/trunk area.
The Consumer Product Safety Commission (CPSC) is a governmental organization tasked with protecting consumers and families from dangerous products and working to ensure the safety of consumer products. They are considered the gold standard when it comes to checking product safety, especially by brand. The CPSC also sets consumer use guidelines for products like trampolines.
Here are some suggested safety guidelines for children using trampolines, and you can find the CPSC’s full set of trampoline recommendations on their website.
- Use a trampoline net enclosure to prevent falls.
- Ensure that trampoline padding covers all frames, hooks and springs.
- Strictly prohibit children younger than six from jumping on trampolines over 20” tall.
- Do not buy or use a ladder for your trampoline in order to prevent children under six from accessing ladders.
- Closely supervise children at all times.
Obviously, part of the fun of jumping on a trampoline for kids is playing with their friends. And while in an ideal world the safest way to jump is one [child] on, one off at a time, we as parents know that’s not realistic. When children jump together try to make sure the children on the trampoline are similar ages in age and size. To accomplish this, consider having the children take turns or jump in shifts with another fun activity planned for those waiting for their turn on the trampoline.
An alternative to consider to backyard trampoline jumping is indoor trampoline parks, which can be found in many cities and offer a somewhat safer option to expel energy while still having fun. Indoor trampoline parks can put kids at risk just like outdoor trampolines would, but actually tend to have relatively low injury rates overall. According to Forbes.com these facilities actually have less frequent injuries than more common forms of kid recreation like baseball, soccer and football.
Most outdoor activities involve human bodies in motion, so any outdoor activity can be dangerous under certain conditions. Trampolines can provide fun and exercise for our children as long as we follow proper safety guidelines. Take the time as a parent to be knowledgeable on trampoline precautions, making sure you are familiar with the specific brand or product in use. Educate your kids on how to properly and safely participate in the activity. Have fun jumping!
William T. Chirico Jr., DPT, Cert MDT, Cert DN is a physical therapist with OrthoCarolina Monroe.
This blog was produced in partnership with Charlotte Parent. Click here for the original post and other parenting resources.